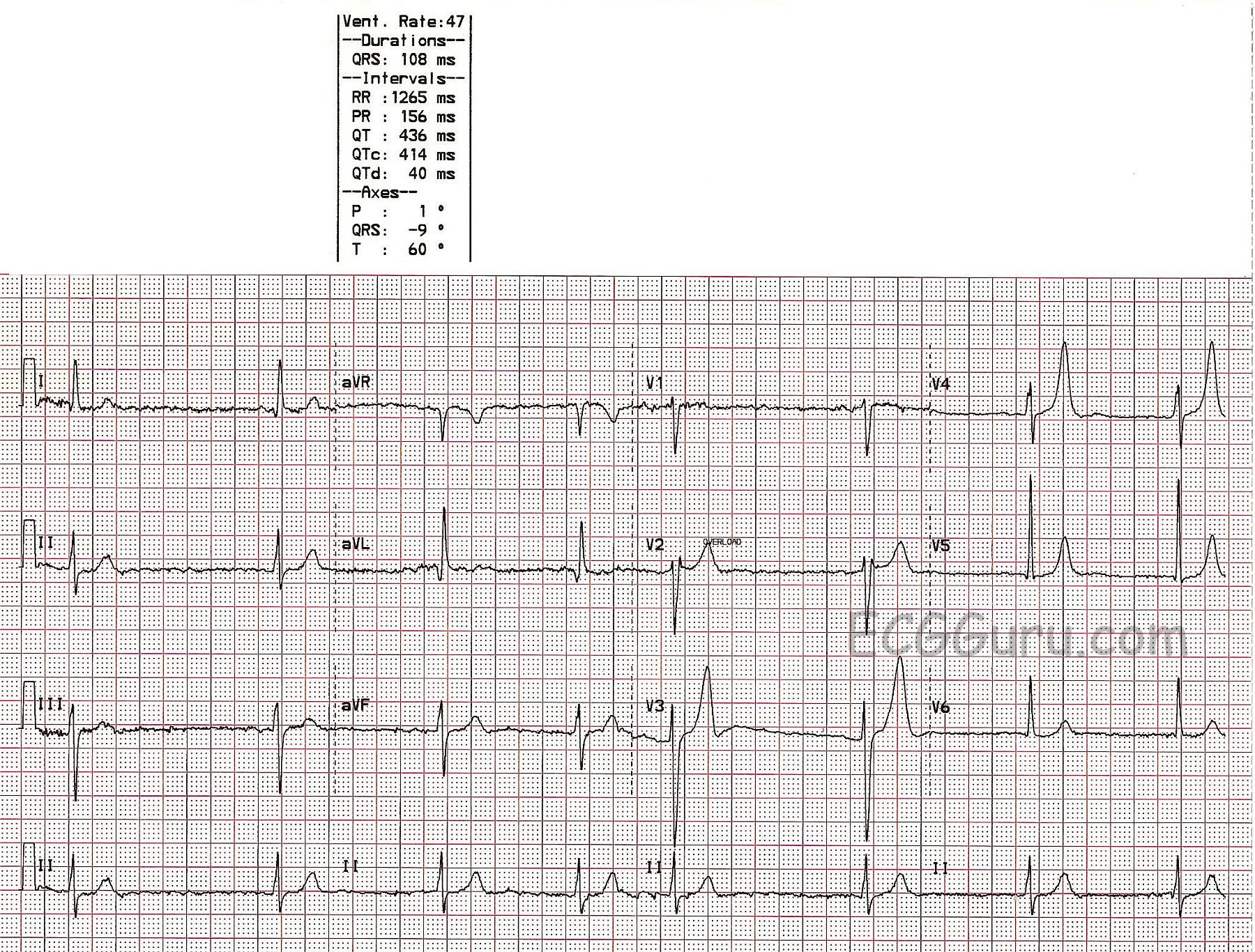
Hypokalemia, a status characterized by abnormally low level of potassium in the blood, can have important implication for cardiac health. One of the critical diagnostic tools employ to evaluate the encroachment of hypokalemia on the mettle is the cardiogram (ECG). Understanding the relationship between ECG in hypokalemia is indispensable for healthcare master to accurately name and contend this condition.
Understanding Hypokalemia
Hypokalemia occurs when the potassium tier in the rake fall below 3.5 mmol/L. Potassium is crucial for maintaining normal nerve function, muscle and nervus action, and overall cellular health. Low potassium levels can lead to assorted symptom, including muscle weakness, fatigue, and in knockout cases, life-threatening cardiac arrhythmia.
Role of ECG in Diagnosing Hypokalemia
The ECG is a non-invasive exam that records the electrical activity of the heart. It is a valuable instrument for find abnormalities in pump cycle and conduction that may be link with hypokalemia. The characteristic changes in the ECG due to hypokalemia include:
- T-wave flattening or inversion: This is one of the earlier signs of hypokalemia on an ECG. The T-waves, which represent the repolarization of the ventricles, become planate or reverse.
- ST-segment slump: The section between the end of the QRS composite and the get-go of the T-wave may be depressed, designate unnatural repolarization.
- U-waves: Prominent U-waves, which are little deflection following the T-wave, can be understand in hypokalemia. These waves are normally not visible but become salient when potassium tier are low.
- Prolonged QT separation: The QT separation, which represent the time from the commencement of the Q-wave to the end of the T-wave, may be extend. This can increase the risk of ventricular arrhythmia.
- Arrhythmias: Stark hypokalemia can conduct to assorted arrhythmia, include atrial fibrillation, ventricular tachycardia, and ventricular fibrillation.
Interpreting ECG Changes in Hypokalemia
Interpreting ECG changes in the circumstance of hypokalemia demand a systematic approach. Hither are the step to accurately see an ECG in a patient with suspected hypokalemia:
- Assess the T-waves: Face for flatten or inversion of the T-waves, specially in the precordial trail (V2-V6).
- Evaluate the ST-segment: Check for depression of the ST-segment, which can be pernicious and may require measured mensuration.
- Identify U-waves: Expression for prominent U-waves following the T-waves. These waves are better seen in the precordial track.
- Measure the QT interval: Calculate the QT separation and correct it for heart pace using the Bazett's formula (QTc = QT / √RR). A lengthy QTc interval may point an increase danger of arrhythmia.
- Check for arrhythmia: Aspect for any signs of atrial or ventricular arrhythmias, which can be life-threatening in severe hypokalemia.
🔍 Note: It is crucial to correlate ECG findings with serum potassium degree and clinical symptoms to substantiate the diagnosing of hypokalemia.
Management of Hypokalemia
Erst hypokalemia is name, prompt and appropriate management is crucial to keep complications. The direction strategy include:
- Potassium supplement: Unwritten potassium appurtenance are typically the maiden line of handling for mild to lead hypokalemia. Severe cases may require endovenous potassium replacement under near monitoring.
- Identify and handle the underlying effort: Hypokalemia can be do by several factors, including diuretic use, gastrointestinal loss, and endocrine disorders. Handle the underlying cause is essential to forestall return.
- Monitor ECG and electrolytes: Regular monitoring of ECG and serum potassium level is necessary to assess the reaction to intervention and prevent complications.
- Avoid triggers: Patient should avoid ingredient that can exacerbate hypokalemia, such as overweening use of diuretic, laxative, or liquorice.
Case Studies and Examples
To instance the importance of ECG in hypokalemia, let's consider a few lawsuit studies:
Case Study 1: Mild Hypokalemia
A 45-year-old patient present with musculus impuissance and fatigue. The ECG shows drop T-waves and mild ST-segment slump. Serum potassium level is 3.0 mmol/L. The patient is begin on oral potassium appurtenance, and the symptoms resolve within a few days. Follow-up ECG testify normalization of T-waves and ST-segment.
Case Study 2: Severe Hypokalemia
A 60-year-old patient with a chronicle of diuretic use nowadays with palpitations and vertigo. The ECG exhibit prominent U-waves, T-wave inversion, and a drawn-out QT interval. Serum potassium level is 2.5 mmol/L. The patient is admitted to the infirmary for intravenous potassium replacement and cardiac monitoring. The arrhythmias declaration, and the ECG normalizes with intervention.
Case Study 3: Hypokalemia with Arrhythmias
A 70-year-old patient with a story of inveterate kidney disease present with syncope. The ECG shows atrial fibrillation with a rapid ventricular response and striking U-waves. Serum potassium level is 2.8 mmol/L. The patient is brace with endovenous potassium and antiarrhythmic medication. The arrhythmia convert to sinus rhythm, and the ECG renormalise with handling.
Preventing Hypokalemia
Preventing hypokalemia involves identifying and manage hazard factors. Some prophylactic quantity include:
- Adequate potassium intake: Ensure a balanced diet rich in potassium, include fruits, vegetables, and whole grain.
- Monitor diuretic use: Regularly monitor potassium level in patients direct diuretics and correct the dose as needed.
- Avoid extravagant laxative use: Boundary the use of laxative, which can cause gi losses of potassium.
- Manage underlying conditions: Properly manage weather that can take to hypokalemia, such as diabetes, aldosteronism, and gastrointestinal upset.
🔍 Tone: Veritable monitoring of serum potassium levels and ECG in high-risk patients can facilitate detect and grapple hypokalemia early.
Conclusion
Hypokalemia is a mutual electrolyte disorder that can have important cardiac manifestations. The ECG play a important persona in diagnosing and contend hypokalemia by detecting characteristic modification in the electrical activity of the heart. Prompt identification and intervention of hypokalemia are indispensable to prevent life-threatening arrhythmia and other complication. Healthcare professionals should be vigilant in monitoring serum potassium stage and ECG in patients at peril for hypokalemia to ensure timely intervention and optimum outcomes.
Related Terms:
- ecg changes with hypokalaemia
- u waves in hypokalemia
- drug causing hypokalaemia
- ecg signs of hypokalemia
- hypokalemia ecg alteration mnemonic
- drugs that cause hypokalemia